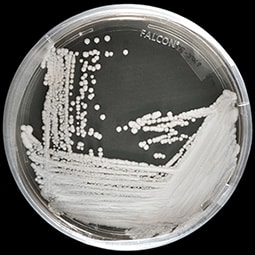
The fungus Candida auris (C. auris) is now considered an urgent threat in the United States after it has spread at an alarming rate in healthcare facilities across the country, but above all, due to its high resistance to antifungals.
According to data published by the Centers for Disease Control and Prevention ‒CDC, for its acronym in English‒ is equally worrying the tripling in 2021 of the number of cases resistant to echinocandins, the most recommended antifungal drug for the treatment of Candida auris infections.
In general, this fungus is not a threat to healthy people, the CDC said in a statement. However, people who are very sick and have invasive medical devices or prolonged or frequent stays in health care facilities are at higher risk of contracting C. auris.
CDC has designated C. auris as an urgent AR threat because it is often resistant to multiple antifungal drugs, spreads easily in healthcare settings, and can cause serious infections with high mortality rates.
"The rapid increase and geographic spread of cases is concerning and emphasizes the need for continued surveillance, expanded laboratory capacity, more rapid diagnostic testing, and adherence to proven infection prevention and control practices," said CDC epidemiologist Meghan Lyman, lead author of the paper.
C. auris has been widespread in the United States since it was first reported in 2016, with a total of 3,270 clinical cases—in which infection occurs—and 7,413 detected cases—in which the fungus is detected but does not cause infection—reported as of December 31, 2021.
Clinical cases have increased each year since 2016, with the most rapid increase occurring during 2020-2021, while the CDC has continued to see an increase in case counts for 2022.
During 2019-2021, 17 states identified their first case of C. auris. Nationwide, clinical cases increased from 476 in 2019 to 1,471 in 2021. Detection cases tripled from 2020 to 2021, for a total of 4,041. Detection is important to prevent the spread by identifying patients carrying the fungus so that infection prevention controls can be used.
C. auris case counts have increased for many reasons, including poor overall infection prevention and control practices in healthcare facilities, as well as increased case detection efforts.
The timing of this increase and findings from public health investigations suggest that the spread of C. auris may have worsened due to pressure on healthcare and public health systems during the COVID-19 pandemic.
CDC’s Antimicrobial Resistance Laboratory Network, which provides nationwide laboratory capacity to rapidly detect antimicrobial resistance and inform local responses to prevent spread and protect people, provided some of the data for the report.
CDC said it has worked to significantly strengthen laboratory capacity, including at state, territorial and local health departments, through supplemental funding supported by the American Rescue Plan Act.
Efforts include increasing C. auris susceptibility testing capacity from seven regional laboratories to more than 26 laboratories nationwide.
You may be interested in: Californians will pay $30 for insulin after contract with pharmaceutical CIVICA

