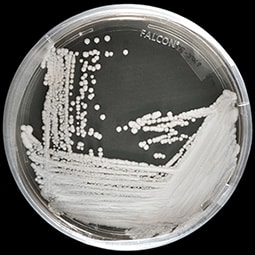
El hongo Candida auris ‒C. auris‒, ya es considerado una amenaza urgente en EE. UU. luego de que este se ha propagado a un ritmo alarmante en los centros de atención médica en todo el país, pero, sobre todo, por su alta resistencia a los antimicóticos.
Según datos publicados por los Centros para el Control y la Prevención de Enfermedades ‒CDC, por sus siglas en inglés‒ es igual de preocupante la triplicación en 2021 del número de casos resistentes a las equinocandinas, el medicamento antimicótico más recomendado para el tratamiento de las infecciones por Candida auris.
En general, este hongo no es una amenaza para las personas sanas, detallaron los CDC en un comunicado. Sin embargo, las personas que están muy enfermas y tienen dispositivos médicos invasivos o estadías prolongadas o frecuentes en centros de atención médica tienen un mayor riesgo de contraer C. auris.
CDC ha considerado el C. auris como una amenaza AR urgente, porque a menudo es resistente a múltiples medicamentos antimicóticos, se propaga fácilmente en los centros de atención médica y puede causar infecciones graves con altas tasas de mortalidad.
«El rápido aumento y la propagación geográfica de los casos son preocupantes y enfatizan la necesidad de vigilancia continua, capacidad de laboratorio ampliada, pruebas de diagnóstico más rápidas y cumplimiento de la prevención y el control de infecciones comprobadas», señaló la epidemióloga de los CDC, Meghan Lyman, autora principal del artículo.
C. auris se ha propagado en los Estados Unidos desde que se informó por primera vez en 2016, con un total de 3 mil 270 casos clínicos ‒en los que hay infección‒ y 7 mil 413 casos de detección ‒en los que se detecta el hongo pero que no causan infección‒ informados hasta el 31 de diciembre de 2021.
Los casos clínicos han aumentado cada año desde 2016, y el aumento más rápido se produjo durante 2020-2021, mientras que los CDC ha seguido viendo un aumento en el recuento de casos para 2022.
Durante 2019-2021, 17 estados identificaron su primer caso de C. auris. A nivel nacional, los casos clínicos aumentaron de 476 en 2019 a mil 471 en 2021. Los casos de detección se triplicaron de 2020 a 2021, para un total de 4 mil 041. La detección es importante para prevenir la propagación al identificar a los pacientes portadores del hongo para que se puedan usar controles de prevención de infecciones.
Los recuentos de casos de C. auris han aumentado por muchas razones, incluidas las malas prácticas generales de prevención y control de infecciones en los centros de atención médica, además del aumento de los esfuerzos mejorados para detectar casos.
El momento de este aumento y los hallazgos de las investigaciones de salud pública sugieren que la propagación de C. auris puede haber empeorado debido a la presión sobre los sistemas de salud y de salud pública durante la pandemia de COVID-19.
La Red de Laboratorios de Resistencia a los Antimicrobianos de los CDC, que brinda capacidad de laboratorio a nivel nacional para detectar rápidamente la resistencia a los antimicrobianos e informar las respuestas locales para prevenir la propagación y proteger a las personas, proporcionó algunos de los datos para el informe.
Los CDC detallaron que han trabajado para fortalecer significativamente la capacidad de los laboratorios, incluso en los departamentos de salud estatales, territoriales y locales, a través de fondos complementarios respaldados por la Ley del Plan de Rescate Estadounidense.
Los esfuerzos incluyen aumentar la capacidad de pruebas de susceptibilidad para C. auris de siete laboratorios regionales a más de 26 laboratorios en todo el país.
Te puede interesar: Californianos pagarán $30 por insulina tras contrato con farmacéutica CIVICA

